Radiological Evaluation of First Trimester Obstetrical Ultrasound
Ask most residents about how they feel about pelvic ultrasound and I think you'll get a " uhh yeah.... I'm okay at it". In reality I suspect most residents don't feel comfortable with it at all and my guess is that the sonographer's worksheet comes in VERY handy. I used to joke that one didn't really get decent at reading US until you completed training (and even then you had the worksheet to fall back on ).
What's the purpose?
The primary purpose is confirmation of an intrauterine gestation. With that we can:
- Evaluate if everything is proceeding "normally", estimate gestational age and predict date of delivery
and more importantly...
- Effectively rule out ectopic pregancy (which is often our primary goal with these exams)*
* While yes, there is the rare chance that this could be a heterotopic pregnancy (ie dual pregnancy where one is inside the uterus and one is outside), the risk of natural heterotopic pregnancy is fairly low (est 1:30,000 - Reference). This risk is elevated (perhaps 10x's) in the setting of ovulation induction therapy. So of course you should look for paraovarian/pelvic masses, but absent these, the presence of a gestation in the uterus is generally considered to exclude the possibility of ectopic/heterotopic pregnancy.
Work-up
There are typically 3 questions that I ask myself in the evaluation of the first trimester Ultrasound.
1. Is the patient pregnant?
This should be the first question one should ask when any young female presents with any pelvic/gynecological symptoms.
The urine pregnancy test (UPT) is the quick and easy answer, however as we will see later, a serum bHCG level can be helpful down the road in the work-up (however seems to be used more and more commonly for diagnosis of pregnancy*).
*Note: if only using a serum bHCG level, very low positive levels can be seen with NON-pregnancy conditions such as pituitary dysregulation, paraneoplastic syndromes and "phantom" pregnancies where low level bHCG can persist following miscarriage. This is always something to keep in mind for very low bHCG levels (say <50mIU/ml). In these settings the UPT can be helpful to confirm actual current pregnancy.
2. Do we see an Intrauterine pregnancy?
Here is where imaging gets involved. First and foremost we are looking for an intruterine gestational sac, ie spherical, simple fluid-filled sac within the endometrial canal. But how can we be certain it is a gestational sac and not just some fluid or blood in the canal? Look for:
- double decidua sign
- yolk sac
- fetal pole
These findings are confirmatory for an IUP. Sometimes the double decidual reaction can be tough to appreciate for multiple reasons, so if unsure, you can fall back to the yolk sac or fetal pole, which usually are pretty easily distinguished, albeit a few days later.
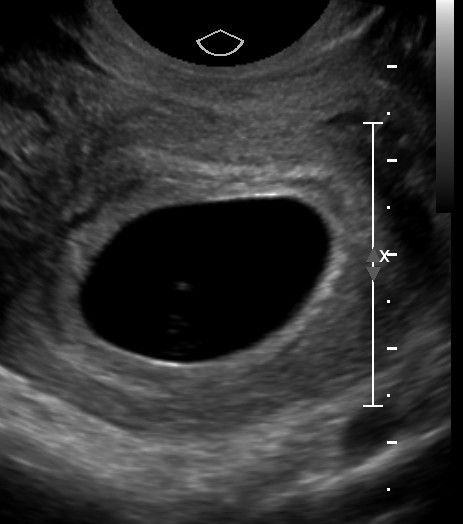
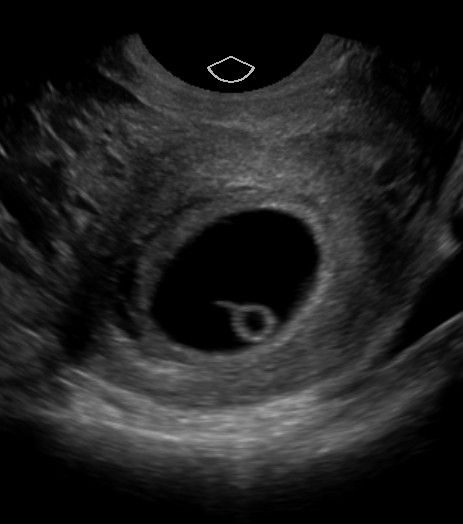
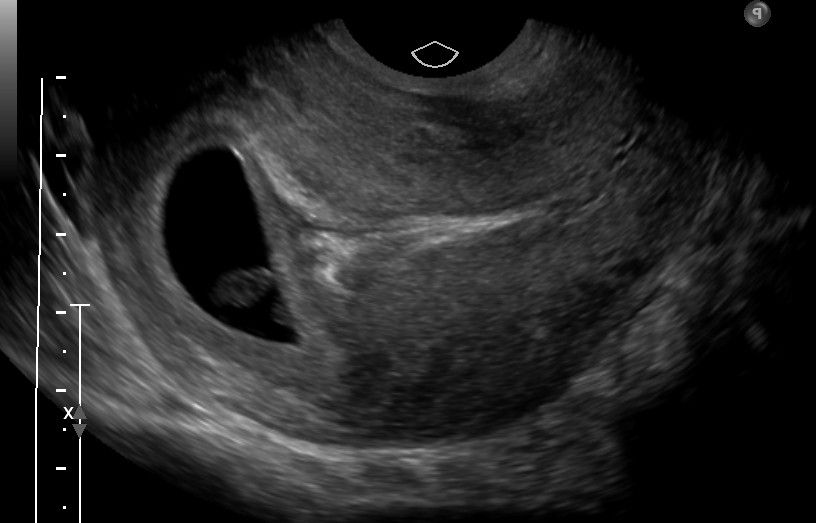
Left: Double Decidual Sign = concentric hyperechoic rings (fairly easy to see in this 7wk pregnancy)
Middle: smaller echogenic sphere/ring within the gestational sac
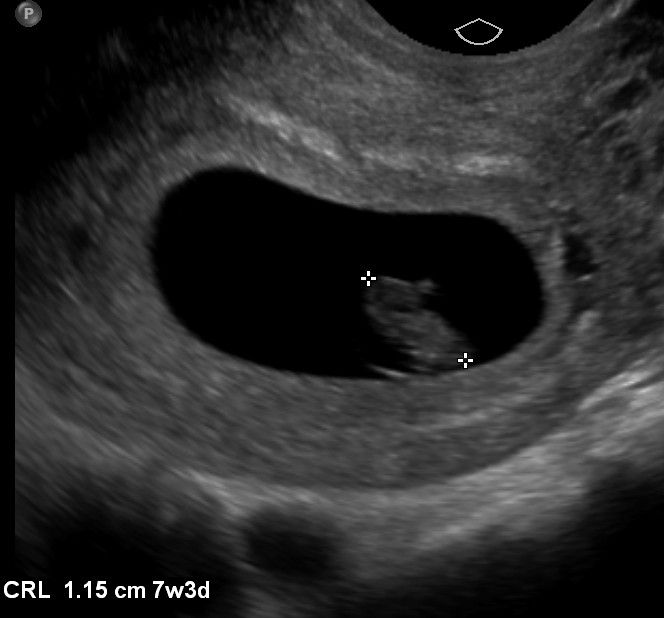
Right: oblong echoic fetal pole should be adjacent to the yolk sac*
*(remember, when you Doppler a proposed fetal pole, M-Mode Doppler only! Color and especially Power Doppler Doppler theroetically could inhibit cardiac function!)
3. Should we see an IUP?
So we have a pregnant patient and we see an IUP. Question answered! YAY! (of course make sure the rest of the exam is normal! but you are otherwise done.)
But what if we have a pregnant patient but we do NOT see an IUP.
To answer this question we need to have an idea of how far along the gestation is - ie Should we see an IUP? For this we can use the serum bHCG level. Studies from long ago have given us the bHCG levels at which for a single gestation pregnancy we should see an IUP:
transabdominally: bHCG = ~2000 mIU/ml
transvaginally: bHCG = ~1200 mIU/ml
So above these levels we should see evidence of and intrauterine gestation and thus these levels are called the discriminatory values.
While these levels have been used for many years and have probably been burned into many brains, in 2018 ACOG (American College of OB/GYN) released an update (below) raising their suggested descriminitory cut-off value to 3500 mIU/ml. Why? My presumption is due to increasing numbers of ectopic pregnancies that were initially treated with methotrexate (which obviously is a teratogen) that later turned out to be just very early intrauterine pregnancies. Remember that standard bHCG doubling time is every 48hrs so we are talking a matter of 36-48 hrs and nature doesn't always fit in our narrow range of normal.
So suggested NEW LEVEL: 3500mIU/ml
ACOG Practice Bulletin No. 191: Tubal Ectopic Pregnancy
Putting this all together
So lets walk through some scenarios
- Pregnant female, no IUP on imaging (and no worrisome pelvic mass, ie identified ectopic pregnancy), and bHCG levels are (+) but < descriminatory value cut-off (ie 3500 mIU/ml). So we don't know where we are chronologically in the pregnancy and we don't know that we should even see an IUP. Options are the so-called triple rule-out, now termed Pregnancy of Unknown location. This includes:
- Miscarriage - could the patient have had an IUP and it passed? (bHCG levels were high and are now decreasing)
- Very early IUP - maybe it's just to small to see (bHCG levels should be increasing)
- Ectopic pregnancy (bHCG levels should be increasing)
OR
- Pregnant female, no IUP on imaging, with bHCG > descriminatory value
- We have rulled OUT IUP. We should have seen an IUP at these levels assuming it was a single gestation!
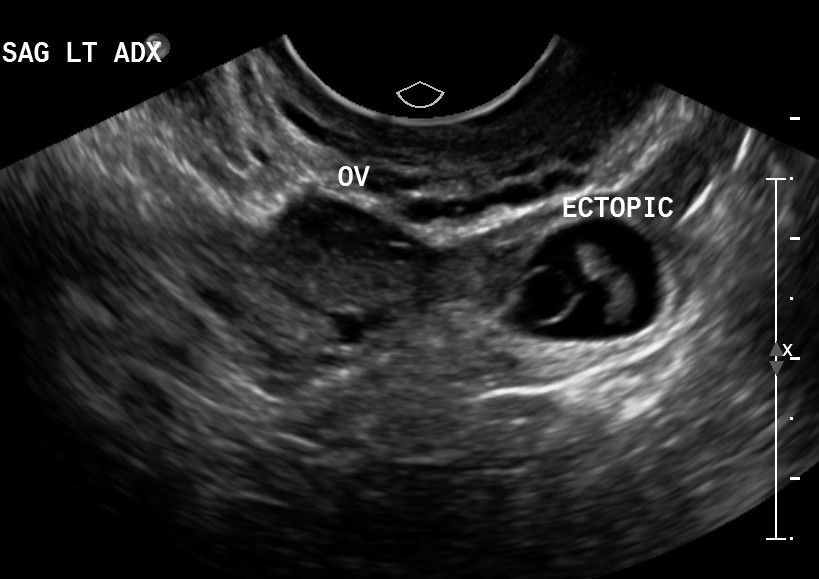
- Ectopic pregnancy - look for hemorrhage, look for a mass in the Fallopian tubes or along the ovary or even in the wall of the uters (isthmic). Once again, yolk sac or fetal pole are confirmatory! but often you don't ever see one. You don't have to see it for it to be present. Clinically bCHG levels should be continuing to rise
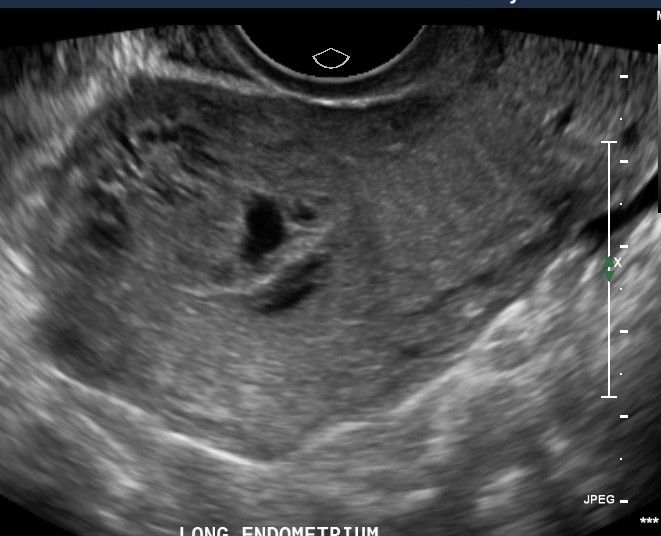
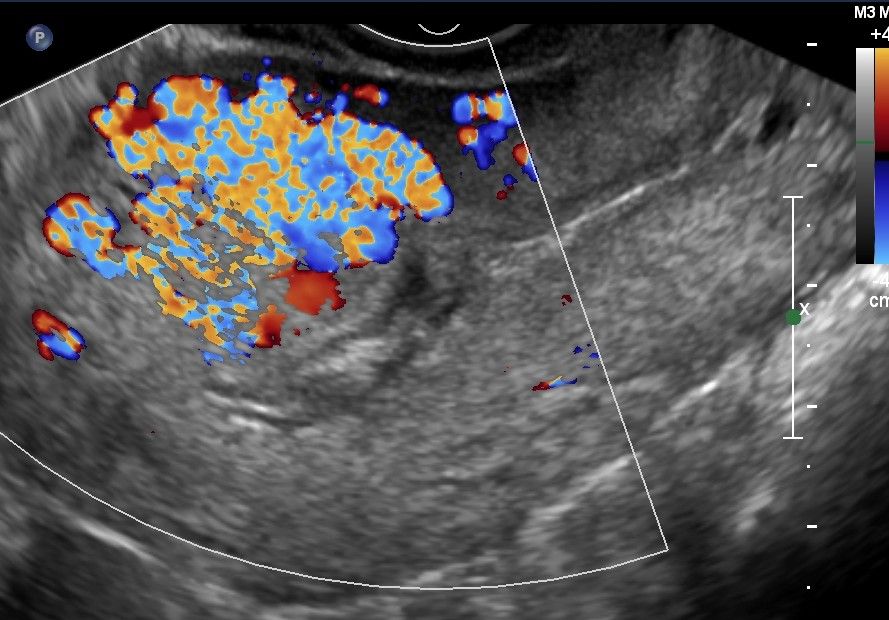
- Miscarriage - Again, the gestation started and has now aborted. bHCG levels should be trending down. Look for complex fluid (blood) in the endometrial canal which can be normal, but always interrogate with Doppler US. If you see vascularity within the cavity = retained products of conception and call your friendly neighborhood OB/GYN as evacuation may be necessary.
*Don't forget, multigestation pregnancies do not have to follow the expected bHCG curves as single gestations, so these are always a bit of a confounder.
**And always remember, particularly in the absence of an IUP, hemoperitoneum (ie blood in the pelvis) in a pregnant patient is ALWAYS concerning for ruptured ectopic. A quick scan in Morrisons pouch up around the liver can help you estimate how much hemorrhage is present. It is at which point I'm usually calling the doc while we are rolling the patient back to the ER as they can decompensate fairly rapidly and that is not good for anyone.
Hopefully now you are less confused! But if not, maybe this flow chart will help.
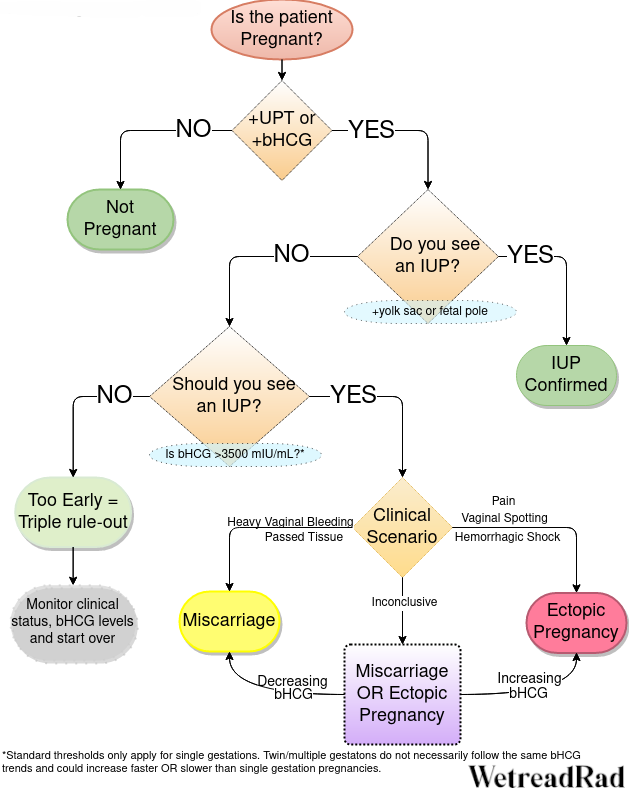
I've just tried to focus on the pregnancy/ectopic work-up because in my experience that mixes up a lot of people. Of course there are all kinds of other pathology to look for, such as:
- subchorionic hemorrhage
- twin pregnancy (see above as double times can be faster or slower)
- anembryonic pregnancy (aka blighted ovum) - where you have a gestational sac but no fetal pole development
- molar pregnancy
- various non-obestrical uterine and ovarian pathology
But I will leave those for another Not so Deep Dive or perhaps some cases :)
See, there is nothing to be afraid of. Pick up that next pelvic US from the ER with confidence!.... and look at that sonographer worksheet to confirm what you see, not tell you what you see.