Season 10 Case 23
Hx: MVA
Would you like more images?
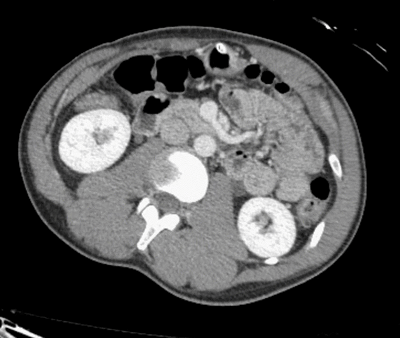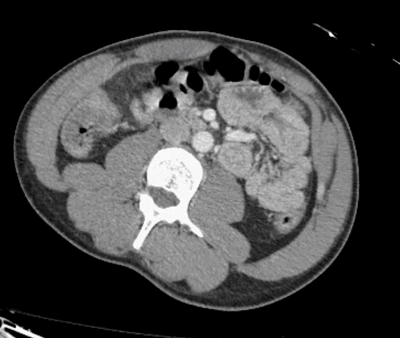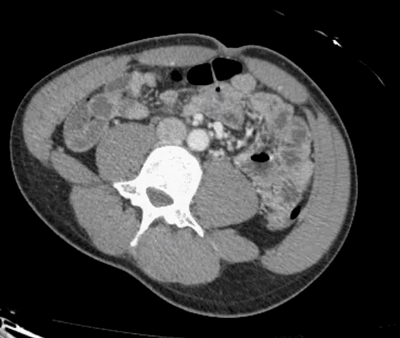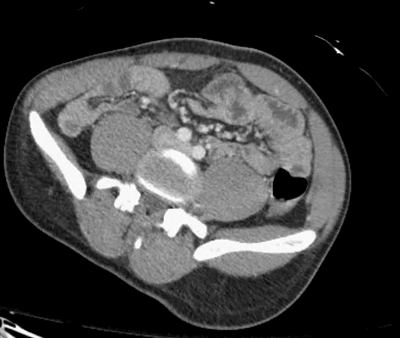
Is there just a single finding, or are there multiple findings?
Answer:
CLICK HERE FOR ANSWER
Transient Intussusception
An intussusception is when a segment of bowel is pulled either into itself or into an adjacent bowel loop due to peristalsis.
Classic teaching is there there is a "lead point", such as a mass, that gets "caught" by the normal bowel peristalsis. The peristalsis then pulls the mass and proximal bowel wall (aka intussusceptum) down through the more distal bowel (intussuscipiens) much like how food normally transits through the bowel.
Although the most common location of intussusceptions is ileocolic (ie distal ileum telescoping into the colon), they can occur anywhere (although gastric involvement is extremely rare).
- Entero-enteric (small bowel into small bowel)
- Entero-colonic (small bowel into colon - see above)
- Colo-colonic (colon into colon)
As one can imagine, this can lead to severe complications:
- bowel obstruction
- as the mesentery gets pulled in it can cause venous/arterial compromise -> bowel wall edema, ischemia and even necrosis
Although "Lead points" are often found in adults, they are infrequently found in children. Possibile lead points include but are not limited to:
- Tumor
- benign (such as polyp, lipoma, GIST, mucocele)
- malginant (such as colon cancer, lymphoma, metastatic disease)
- Developmental
- Meckel's diverticulum
- duplication cyst
- Hypertrophic Peyer's patches (GI lymphoid tissue)
- Thought to be the the most common cause in children (not usually visualized macroscopically)
- Thought to be the the most common cause in children (not usually visualized macroscopically)
Clinical findings of pathologic intussusception
Classic findings include:
- intermittent abdominal pain
- vomiting
- Right upper quadrant "sausage-shaped" mass
- occult or gross rectal bleeding
- classic description is "currant jelly stool" *this is concerning for undeerlying bowel ischemia/necrosis
- classic description is "currant jelly stool" *this is concerning for undeerlying bowel ischemia/necrosis
Radiology
X-ray
- elongated soft tissue mass with proximal dilated bowel loops (ie bowel obstruction)
Flouroscopy
-
similar findings as X-ray, but after giving oral contrast, the classic finding is the "coiled spring" appearance where you see oral contrast both within the lumens of the intussusceptum and intussuscipiens.
-
The benefit of flouroscopy is real time imaging and the ability to perform interventions. In children this allows for real time reduction of the intussusception using air (or water soluble contrast) administered rectally. By creating a retrograde backpressure, one can "push" the intussuscepting loop backwards out of the intussuscipiens.
-
Of course this should NOT be attempted if there is any concern of ischemia/necrosis (bloody/ currany jelly stool) or perforation (peritoneal signs, free air, etc)
Ultrasound
Ultrasound can be highly sensitive and specific and is ideal for children given it's lack of radiation. Look for:
- Target sign (aka bullseye sign) = rings of hyper- and hypo- echoic circles correlating to the alternating cross-sectional layers of mucosa (hyper-), submucosa (hypo-), and muscularis (hyper-) of the intussusceptum (inner layers) out through the intussuscepiens (outer layers)
- Peudokidney sign = longitudinal appearance of the intussuscepted loop within the lumen of the intusscepiens
CT
The modality of choice in adults.
When imaged in transverse cross-section, the appearance mimics the target (aka bullseye) sign above, showing the wall of the intusscepted loop, surrounded by the wall of the intussuscpiens.
When imaged longitudinally, one can actually see the bowel loop telescoping into the intussuscipiens in longitudinal cross-section.
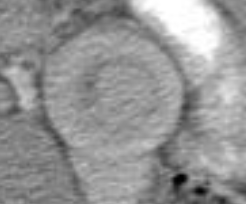
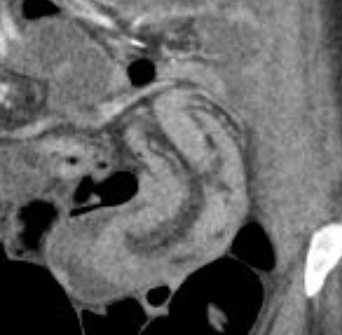
Left: concentric bowel-within-bowel rings of the Target Sign. On the right we see the the longitudinal cross-section of one bowel loop pulled into another with mesenteric fat between the bowel walls
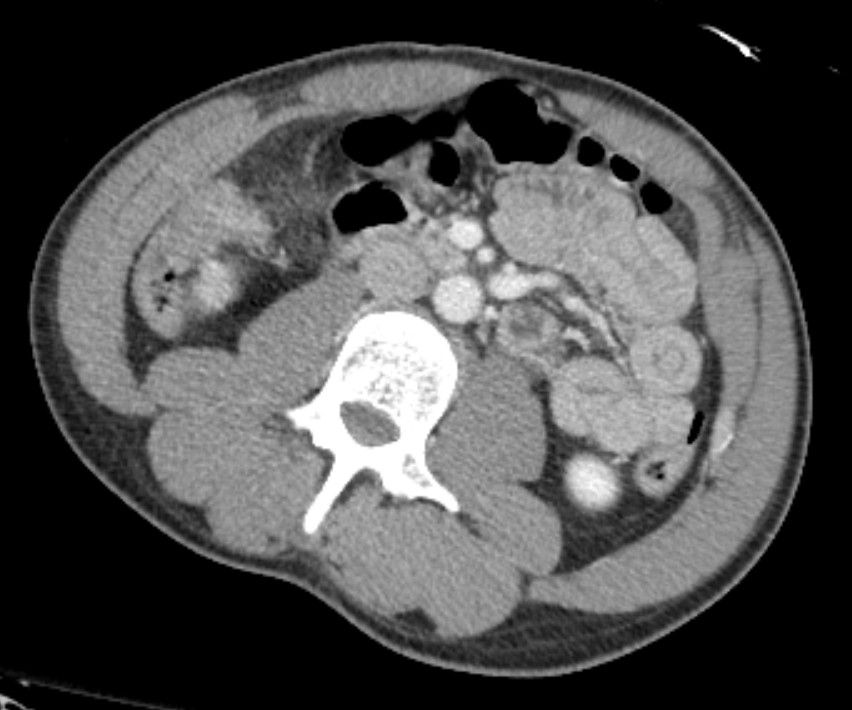
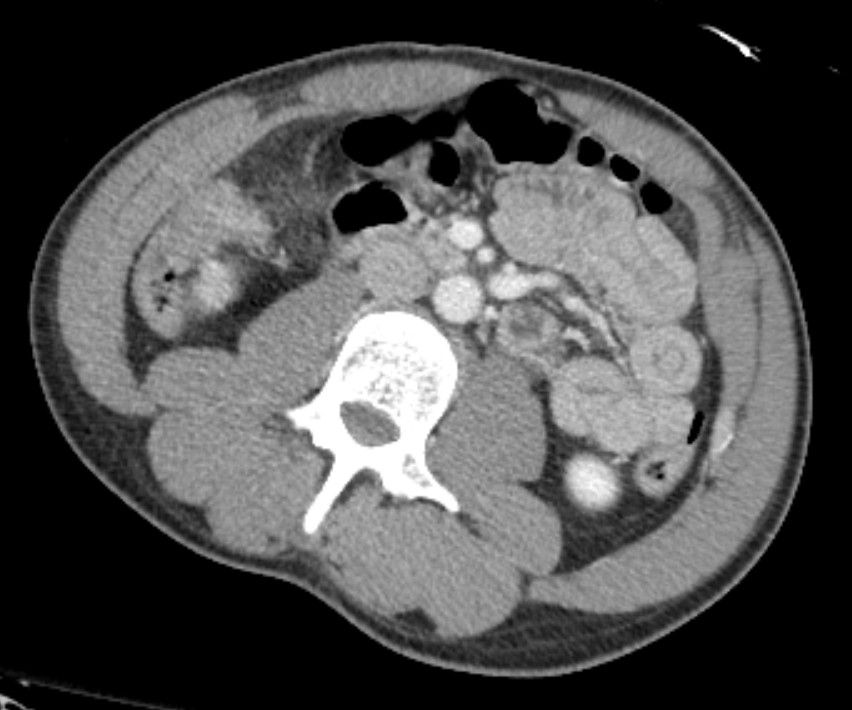
Back to our case.
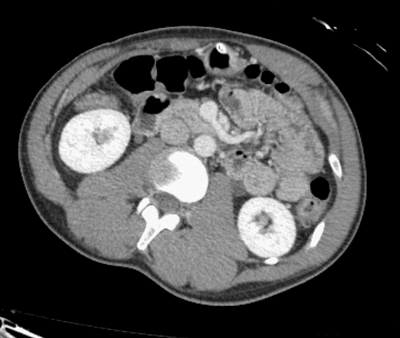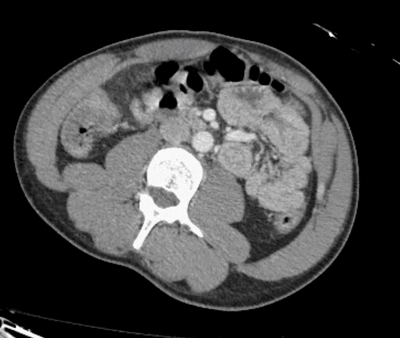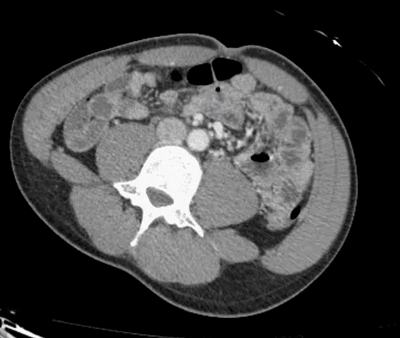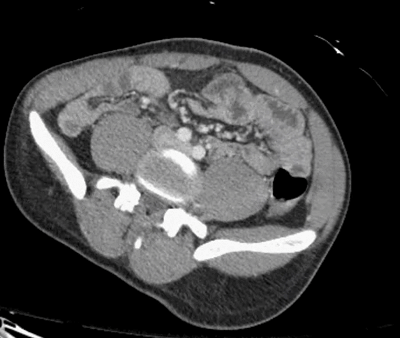
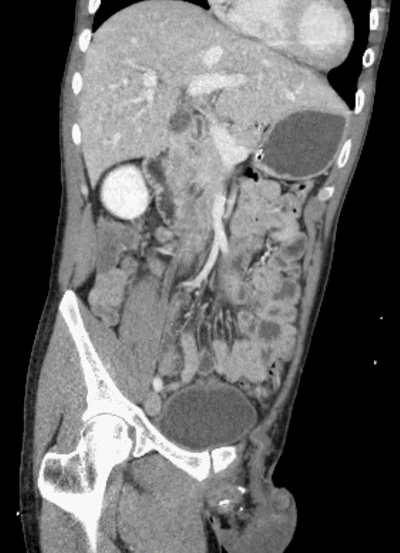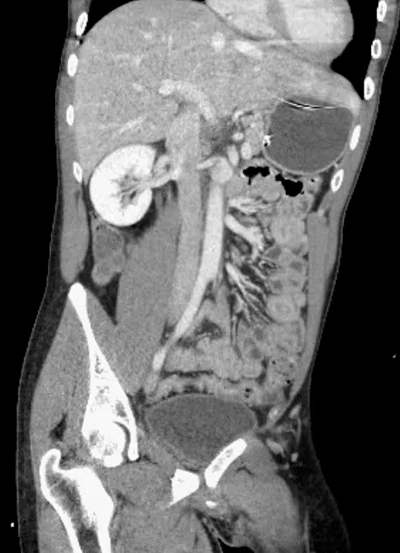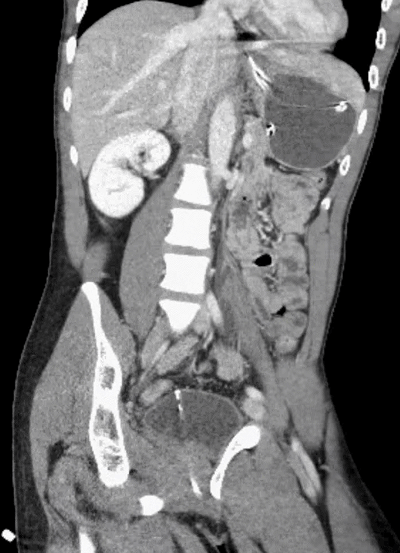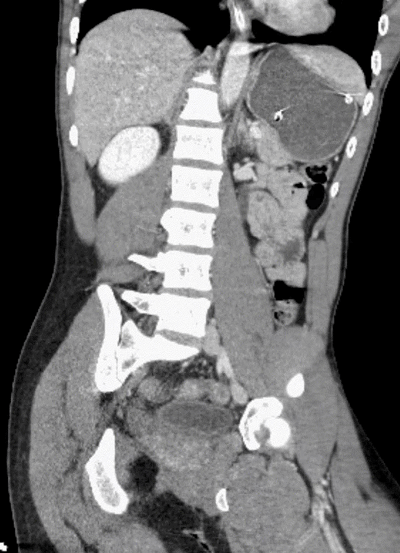
Did you find the intussusception? Did you perhaps find more than one?
I think I stopped counting at SIX instussecptions in this completely asymptomatic patient being scanned after an MVA (they had other significant extremity injuries). Are there even more?
Transient Instussusception
While all of the above is true, that all applies to pathologic intussusceptions. Here we have NO bowel dilation/obstruction, NO descrete lead points and NO bowel wall edema/hypoenhancement to suggest vascular compromise. Thus these are termed incidental or transient
intussusceptions.
My experience is that these are not uncommon. I can't even count the number of times (nonetheless the number of instussusceptions!) that I have encountered incidentally on asymptomatic patients, often after motor vehicle accidents (correlation? causation? who knows). But again, as long as there was no concerning findings listed above, they have all resolved, even on extremely short term follow up (even within the time between aterial and portal venous imaging!)
While I do tend to mention these in my report, I try to be explicit that they are extremely likely to be transient/incidental in the abscence of symptoms. And if/when the doc calls with concern, you can reassure them that unless the patient has symptoms listed above, they are verly likely to be resolved by the time you are talking.
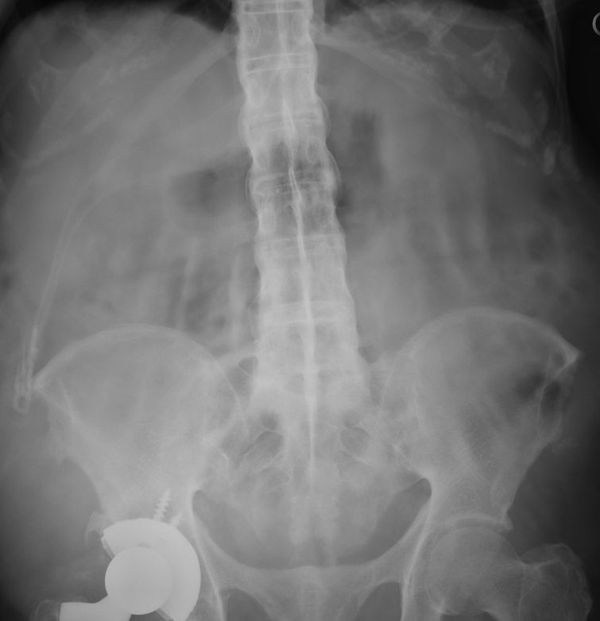
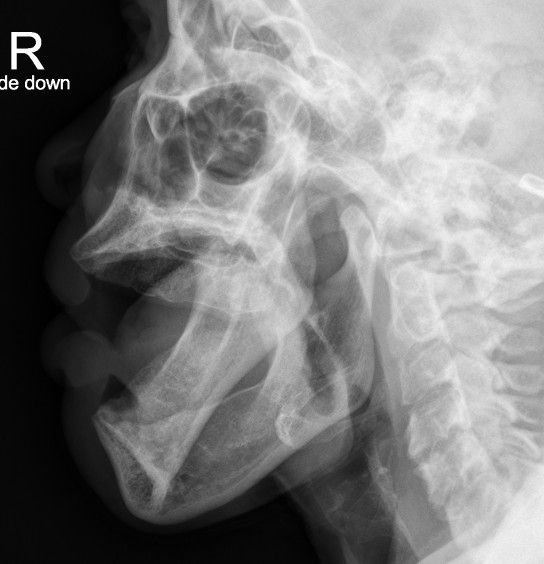
If you'd like to see other examples, feel free to check out some older Wetread case below. The write-ups were much shorter then, but now they you know all about intussusceptions, it's the imaging that is important right?
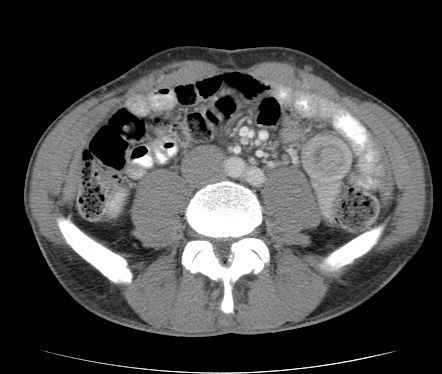
Full size version of Example #1 above
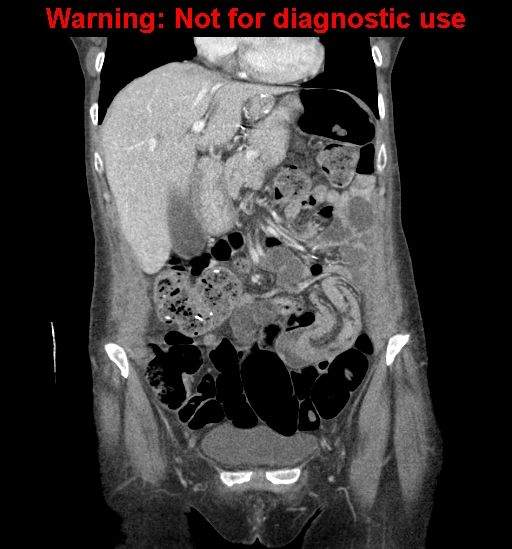
Full size version of Example #2 above